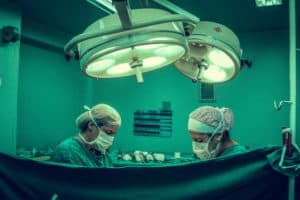
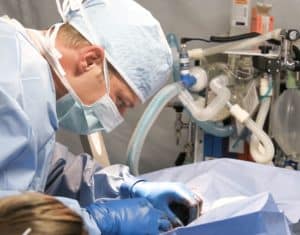
To put it simply, surgical centers are places where outpatient surgeries of all kinds take place. Experts are predicting that the need for these surgical centers will grow in the future, as more and more procedures are able to take place on an outpatient basis. The downside is that the billing process for them is complicated, leading to plenty of possible mistakes that could lead to disaster as commercial insurance companies reject the claims even after appeals.
Surgical Centers Are an Important Part of the Healthcare Market
These surgical centers, according to one expert, are predicted to rise in number. According to David Stack, “the company estimates around 70 percent of surgeries are done in hospitals and 30 percent are done in ASCs; however, over the next 10 years Mr. Stack projects that will flip to 70 percent of surgeries performed in an outpatient or ambulatory setting and 30 percent in the inpatient hospital.” This means that as the number of surgical centers grows, so do the potential billing issues that can lead to things like state-level appeals and Federal ERISA appeals.
The main reason for this future reliance on surgical centers is cost. That same expert stated that “The payers have seen the value of providing improved care at a 40 percent reduced cost [in the ASC]. With the advent of [enhanced recovery after surgery protocols] and physician-owned surgery centers, physicians want to work there and payers want surgeries performed there.” Although the cost for treating patients will go down, the potential for billing issues goes up, especially when you consider the fact that many of these surgical centers are equipped, and will be paid a bit more, for surgeries that take place without opioid painkillers. The complicated billing process is what needs to be worked out for these surgical centers to succeed.
Preventing Billing Issues
Not every billing issue can be prevented, but some certainly can. When a patient has a procedure done, their medical insurance – the commercial health insurance company – is sent a claim from the surgical center. If there are any issues with this claim, such as a wrong date of birth, a misspelled patient name, or even a typo in the patient’s insurance information, then the claim will go unpaid. The complicated billing process doesn’t help this any.
How the Billing Process Works
Like with most billing departments, the ones at these surgical centers have a number of codes that they need to keep track of. Every commercial health insurance company has a contract with the surgical center. This information includes how much the surgical center can bill for certain procedures, as well as how those claims are sent in. Most are sent electronically to the insurance companies, making it easy to track them. The problem comes when mistakes are made in the billing process. Sometimes things end up getting miscoded, or the wrong amount is requested. When those claims are sent back to the surgical center, it’s up to the billing employees to double-check them and then resubmit them. This resubmission is the first of their state-level appeals. Only three are allowed.
In most cases (as you can see from the statistics included above) most claims are paid by the end of the three appeals. The problem comes when they aren’t. No matter the reason for the unpaid or underpaid commercial health insurance claims, these finished appeals can cause a number of problems.
There Are Only Three State-Level Appeals
Every surgical center has three state-level appeals that they go through when trying to collect on a commercial health insurance plan. The ways in which the appeals are done depends on the insurance company itself. Every one of them has a different form, another process, and sometimes a separate address that those claims need to be sent to. This just makes it more difficult for the surgical center’s billing employees. They need to know the specifics and have enough time to deal with each round of appeals. There’s usually a lot of paperwork involved. What makes this even trickier is the time frame.
According to the statistics in Becker’s most of these claims are sent out for payment within three days of the surgery. The time that it takes to wade through the codes and billing documents to find the correct forms is what generally leads to these delays. Without those specifics, the process would move much faster. It gets even worse when you consider what happens when those claims are sent back unpaid or underpaid. You only receive three state-level appeals on these claims before they end up being shelved for good. At that point, they end up in what we call a debt bucket, on the wrong side of the balance sheet. If those add up enough – and the rate of fully paid claims begins to fall precipitously – then your surgical center ends up in financial hot water.
What Happens When Those Bills Go Unpaid
Surgical centers have quite a few bills to pay, including the surgeons and supporting doctors and nurses, their utilities, any building maintenance and upkeep, and necessary supplies. Without a cash flow that consists of 100% paid claims, your surgical center could end up in financial trouble. There’s also the issue of the “boom period” that surgical centers are in. The need and market for them could end up shrinking, making these unpaid claims even more important.
The Federal ERISA Proces
Thankfully, there’s an option when it comes to those rejected surgical center claims – the Federal ERISA appeals process. ERISA, also known as the Employee Retirement Income Security Act, is a method used by specialists to ensure that those commercial healthcare claims get paid. According to ERISA, which was created to govern employee retirement plans and then expanded to include self-paid health insurance, those unpaid commercial healthcare claims must be paid. However, this is a specialized and time-consuming process.
The main issue is that the surgical center billing employees don’t have the time to go through the Federal ERISA appeals process. These billing employees more than likely don’t know how even to begin such an appeal, nor do they have access to complete the paperwork and follow up on them. They’re too busy sending out bills for current claims, as well as dealing with those that are in still working through the state level process. All of that money – which these surgical centers really could use – is going uncollected. You need us, ERISA Recovery, to handle the Federal ERISA appeals for you. We don’t require any payment up front and even have a 12-month $1 million guarantee. To be specific, we guarantee that we’ll collect $1 million in claims for you over a 12-month period, as long as we have access to the information that we need.
You Need Help
It’s time for you to take control of your surgical center’s financial future. You need to ensure that your collection rate from commercial health insurance companies is 100%. This is why you need to contact ERISA Recovery today so that we can help put the Federal ERISA appeals process in motion. You can reach us at (972) 331-4140 or by filling out the contact form on our website.